|
| Dr. Brooks examines a pediatric patient |
If you have had a cat for any length of time, you have probably had to take him or her to the veterinary hospital for something other than an annual checkup at least once - anything from a bite wound from another cat to a broken toenail; stuffy noses, runny eyes or even (every cat owner's nightmare) choosing to urinate outside the litterbox.
Have you ever wondered, while sitting in the exam room waiting for the doctor, what other visitors to the hospital are bringing their cats in for? Veterinary Pet Insurance analyzes their claims each year, which can give us a good idea why most people are bringing their cats in to see the veterinarian. Last year, the top 10 reasons that cats visited the veteirnarian for a health issue were:
 |
| Cancerous cells typical of lymphoma |
9) Upper respiratory infection: Many young cats and kittens visit us because they are sneezing or have a runny nose or watery eyes. Some cats that have been affected by an upper respiratory infection as a young cat may have chronic but fairly manageable problems for the rest of their lives.
8) Inflammatory Bowel Disease: IBD is not a single disease but a complex group of symptoms and conditions that result from increased inflammation in the digestive tract. This condition can cause problems with digestion and absorption of nutrients, susceptibility to bacteria and viruses in the intestinal tract, vomiting, diarrhea, weight loss, poor hair coat, increased production of hairballs and more. For more information, you can read our blog article on IBD, here.
 |
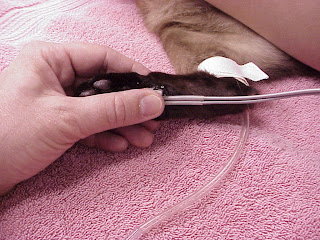
| Drawing up insulin injections for a diabetic cat |
7) Diabetes: Middle-aged to older cats, especially males and overweight cats are at higher risk for diabetes. As the obesity problem in US pets grows, the prevalence of diabetic pets has also increased. Almost 60% of cats are overweight in the United States, according to data collected by the Association for Pet Obesity Prevention (APOP) last year (2014). For more information, you can read our blog article on diabetes, here.
6) Diarrhea or intestinal upset: Sometimes caused by intestinal parasites, diarrhea can be any stool that is soft or not well-formed, whether the cat can make it to the litterbox or not. Other causes of diarrhea may include diseases such as thyroid disease, IBD, or other problems, such as constipation (oddly enough), or eating a non-food item, such as a toy or ear plug.
5) Excessive thyroid hormone: Overactive thyroid glands produce more thyroid hormone than necessary, which can cause symptoms such as increased hunger and thirst, rapid heart rate, hyperactivity, vomiting, diarrhea and weight loss. For more information, you can read our blog article on hyperthyroid disease, here.
4) Vomiting/upset stomach: Vomiting may be related to an underlying medical issue such as thyroid disease, or may be caused by a food allergy, ingestion of a non-food item, a hairball that has become stuck in the digestive tract, heartworm disease, constipation or other problems.
3) Chronic kidney disease: A common problem in older cats is a progressive decrease in kidney function which can cause symptoms such as weight loss, vomiting or nausea, poor appetite. For more information, you can read our blog article on Chronic kidney disease, here.
 |
| Annual oral exams help prevent serious dental disease |
2) Periodontitis/dental disease: About 85% of cats over the age of 3 years have some amount of dental disease. Imagine the state you might be in if you didn't brush your teeth for three years or more! Most cats will need some level of dental care at some point in their lives. Just like people, a lot of a cat's dental health is related to genetics - enamel strength, tolerance of bacteria in the mouth, but regular dental checkups and cleanings can help prevent severe dental disease. For more information, you can read one of our blog articles about dental disease, here.
 |
| Making sure your cat likes the litterbox can help prevent urinary issues |
1) Bladder or urinary tract disease: Just like VIP, the most common reason that we see cats for
medical care at Exclusively Cats is due to bladder or urinary problems - often because the cat has started to urinate outside the litterbox. There are many reasons that a cat might develop litterbox issues, many of which are medical and none of which are due to revenge or spite, despite what many people think or feel. As Dr. Deporter at Oakland Veterinary Referral Service is fond of saying, a cat's urine marking behavior is like leaving a sticky note with important information in a certain area. When we go by and clean up the urine without looking for the root of the problem, we are removing valuable cat information from the spot. This means the cat feels the need to re-post the sticky note - and they will continue to do so until the problem is addressed. The cat can read the "sticky note", other cats can read the "sticky note", but we humans cannot read the "sticky note" and need to use other means to figure out what the cat is trying to tell us. Sometimes it may simply be "Hey! My litterbox is stinky!" other times it may be a different cry for help. For more information, please read the 4 part series of blog articles that we have prepared on bladder and litterbox issues which begins here.